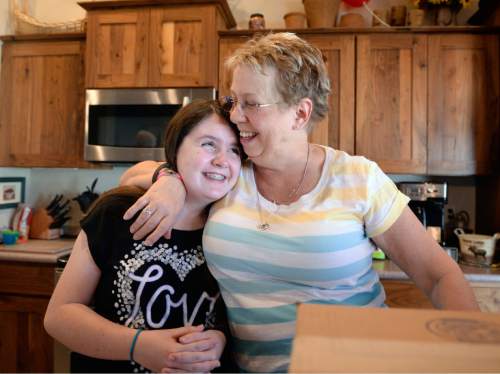This is an archived article that was published on sltrib.com in 2016, and information in the article may be outdated. It is provided only for personal research purposes and may not be reprinted.
Deb Scott looked into the eyes of the woman dying from hepatitis and saw her own future.
A social service aide at a skilled nursing facility, Scott could see that the woman's stomach was bloated with fluid and could hear her cry out in pain.
Scott was healthy at the time, but because she had hepatitis C, she kept that woman in her thoughts. She stopped daydreaming about her retirement or imagining seeing her grandchildren grow up.
"I seriously believed my life would be dramatically shortened by this horrible disease," said Scott, now 63. "I never planned my future. I was told too many times I would not have a future."
Like the 3.5 million Americans with hepatitis C, Scott was elated when, starting in 2013, the Food and Drug Administration approved new antiviral drugs that boasted a hepatitis cure rate of almost 100 percent with few side effects.
But they've proven an elusive cure for many. A full course of treatment can range from $83,000 to $189,000. The hefty price tag has led Medicaid agencies, prisons and private insurers to restrict access to the drugs.
—
—
'Unique in modern medicine'
Hepatitis C is a virus spread through blood-to-blood contact, mainly from sharing needles, and there is no vaccine. The virus affects up to 4 percent of adults in the United States. Michael Charlton, medical director of Intermountain Medical Center's liver transplantation program, says just 2 percent of Utah adults are infected — and most don't know it.
Still, it's the No. 1 reason Utahns need liver transplants. And while a small portion of people are able to defeat the virus via their own immune systems, most will develop a chronic infection that often leads to liver disease and, less commonly, cirrhosis or liver cancer.
Scott believes she got hepatitis when she was hospitalized in the 1970s with a broken jaw. That decade — when intravenous drug use was high, blood products weren't screened for the virus and now-standard universal precautions for how body fluids are handled weren't used — was the height of hepatitis infection.
But the virus has come roaring back because of the exploding levels of abuse of heroin and methamphetamine.
Hepatitis C is Utah's second-most commonly reported communicable disease, after chlamydia and before influenza that results in hospitalization. And Utah's rate has jumped, in part because more are getting tested as they've heard about the wonder drugs.
Previous treatments could cure only up to 50 percent of cases, and included injecting interferon, which caused diarrhea and hair and weight loss.
The new, interferon-free, oral treatments have proven safe and highly effective. The drugs include Sovaldi and Harvoni, both made by Gilead Sciences; AbbVie's Viekira Pack; and Janssen Research and Development's Olysio.
Hepatitis C could go the way of smallpox and disappear if treatment were widely available, said Charlton, who is a member of a national panel that created recommendations on how to manage and treat hepatitis.
"It might even be unique in modern medicine," he said. "You give patients pills for 12 to 24 weeks and those pills will make the hepatitis C virus go away and never come back, if there isn't a new infection down the road."
While treatment was once prioritized for sicker patients, the guidelines now say everyone with a chronic infection — except those with a short life expectancy — should be treated, and treatment should start before patients develop liver disease. Studies show that delaying treatment can increase the chances of liver-related death fivefold.
But many public and private insurers have continued to restrict the drugs to patients with advanced stages of liver disease.
—
Denied treatment
Through the 1990s, Scott tried various combinations of drugs, injecting herself with interferon and living with flu-like symptoms for more than a year. At one point, her liver was heavily scarred and she was close to developing cirrhosis. And while she did improve, she expected her liver to eventually fail.
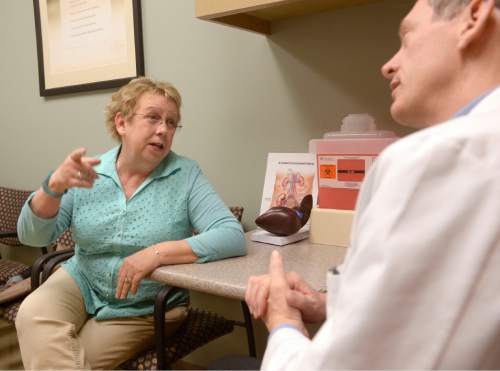
But getting better meant she couldn't take Sovaldi. Scott's private insurer, whom she didn't want to name, told her in 2014 she needed to be sicker to qualify for the treatment. The company refused to cover it, she said, even after her doctor wrote in an appeal that the insurance company would be responsible if she died.
An unknown number of Utahns have been denied treatment. The Utah Insurance Department says it isn't able to tally how many have complained to the agency about hepatitis C coverage problems or the outcomes of those appeals.
But it does track how many complaints proceed to an external review, the final stage of the appeals process. Last year, five cases were reviewed; in three cases insurers were required to provide coverage. The Insurance Department denied a Tribune records request for those findings.
Restrictions on access and the high cost of treatment prompted the U.S. Senate Finance Committee to investigate Gilead's pricing practices. A report issued in December found the manufacturer focused on maximizing revenue even though it knew a lower price would allow more people to be treated.
The committee sought public comment on how to address the problem of the high prices of breakthrough drugs while ensuring patient access. Some ideas included requiring manufacturers to offer higher rebates for such drugs and expediting the approval of generic drugs.
In response, Gilead defended its pricing, noting that the drugs benefit patients and are less costly than the possible long-term effects of the chronic condition such as liver cancer and liver transplants.
All of the large national private insurers surveyed in the investigation required some level of disease severity, and that the restrictions were largely based on reducing costs. In Utah, SelectHealth's prior authorization for Sovaldi requires information about disease severity.
The Senate report also found widespread restrictions among Medicaid agencies and fears among Medicaid managers that the drugs would destroy their budgets. Just a sliver of Medicaid beneficiaries who have the virus, less than 3 percent, got treatment in 2014.
A 2015 study published in the Annals of Internal Medicine found most agencies pay only for patients with advanced liver disease, and some require patients to abstain from drugs or alcohol, contrary to medical guidelines.
That's led to class-action lawsuits by Medicaid beneficiaries in Indiana and Washington, with plaintiffs' attorneys claiming it is illegal to withhold curative drugs based on their cost.
—
Cure or endure
Utah's Medicaid program is different: It says it has approved all requests for hepatitis treatment during the current fiscal year.
It requires minimal prior authorization for the drugs, along with tests to detect the virus and determine its genotype. However, the state doesn't cover the genotyping test.
The Utah Health Policy Project, which advocates for expanded Medicaid coverage, has received no complaints about Medicaid's hepatitis coverage.
But the drugs are taking a bite out of Utah's Medicaid budget.
A year after Sovaldi was approved, it shot to the top of the list of drugs Utah Medicaid spends the most on, outranking medications for much more common conditions such as diabetes and depression. In 2014, the state paid $5.5 million for 66 patients to take the wonder drug.
In 2015, once Harvoni was widely available, it took the No. 2 spot on Utah's list. Gilead's drugs cost Utah Medicaid $9.7 million last year. That's nearly 10 percent of its $102.7 million medication budget, though the actual costs are likely lower because Medicaid gets rebates from drug manufacturers.
Utah has no plans to restrict access, said Emma Chacon, Utah's Medicaid operations director.
"Other states may have a higher percentage of beneficiaries with hepatitis C diagnoses than we do," she said. "Our intention is to continue to provide it as we have without any additional restrictions."
Utah's Department of Corrections, however, limits how many prisoners it treats — spending about $800,000 last year to treat eight prisoners.
Five times as many inmates are in line for the treatment because they meet most of the prison's criteria for care, which includes having enough time left on their sentence (18 months) to finish the treatment, testing negative for drugs for the prior two years, and having consistently abnormal liver lab tests.
Tony Washington, health services administer for Corrections' Clinical Services Bureau, said the 40 to 45 inmates would benefit from the treatment, but there isn't enough money to treat them all in a year. This year, the Legislature allocated $400,000, though the prison will likely spend more than that.
"Most of these inmates are not here for life," Washington said. "They could be treated after they leave prison."
Prisons can and do use budget decisions to dole out care, though demonstrating "deliberate indifference" to serious medical needs is illegal. Attorneys representing prisoners have filed class-action lawsuits against Massachusetts, Minnesota and Pennsylvania for denying access to hepatitis C drugs.
But Utah's chapter of the American Civil Liberties Union could find just three complaints from prisoners since 2013.
As in the Medicaid system, Utah's prison system spends the most money on hepatitis C drugs. "What it would cost to treat one hepatitis C patient, you could probably treat 50 of our more typical chronic care patients [who have diabetes or hypertension] for a year," said Bruce Burnham, a doctor at the prison.
Hepatitis C treatments are straining the U.S. Department of Veterans Affairs medication budget, too. In Utah, the VA spent $4.4 million last year to treat 125 veterans. That's much higher than what it pays for the more commonly used and next most expensive medication, insulin, at $1.75 million in 2015. Congress recently earmarked $1.5 billion to treat veterans for hepatitis C.
—
'So much relief'
Happily for Scott, Intermountain Medical Center was seeking patients like her for a trial of Merck's new antiviral. She joined in 2014 and says that within a month, the amount of virus detected in her blood dropped to zero.
"The doctor described it as an [atomic] bomb going off," she said. "It just obliterated" the virus.
She and her husband recently bought a motor home and are considering living in Texas or Alaska when they retire. "It's a dream come true," she said. "I've had so much relief and so much joy in knowing that I don't have this disease anymore."
The FDA approved the drug Scott used, named Zepatier, earlier this year. Its list price of $54,600 for a 12-week course was heralded as a game changer. Zepatier is expected to eventually help lower costs across the industry as Gilead and others are forced to compete.
"Maybe I contributed just a teeny bit to one more drug being on the market that will help a lot of people. I hope so," Scott said. "It would be such an easy disease to get rid of."
Intermountain Medical Center was involved in a recent trial of another Gilead hepatitis drug that Charlton says will advance medicine again.
The company's latest product could simplify treatment because it covers all genotypes of the virus. The company submitted an application to the FDA in October to combine Sovaldi with a drug that inhibits the replication of the virus. The treatment has proven effective even for people with liver failure, improving liver function for half the patients.
"We were able to cure people who had life-threatening liver failure," said Charlton, a co-principal investigator in the study.
He sympathizes with patients who want to be cured and with the drug companies who want a return on their investment, noting that the development costs of Sovaldi "exceeded $11 billion."
"As a doctor, I would like to treat any illness that a patient I'm seeing is suffering from. But we also live on planet Earth," he said. "Sometimes treatments are expensive."
In time, he said, costs will come down. And in many cases, time is on the patient's side. "Luckily," Charlton said, "it's a slow illness. It's a disease of decades." —
Tell the Tribune
O Have you been able to access hepatitis C treatment? › sltrib.com/upin