This is an archived article that was published on sltrib.com in 2011, and information in the article may be outdated. It is provided only for personal research purposes and may not be reprinted.
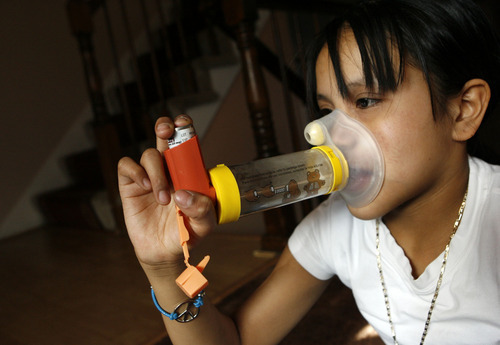
Karina Contreras vividly remembers watching her daughter's parched lips turn purple and the rapid rise and fall of her stomach as she battled to breathe.
Between the ages of 1 and 3, Karime was hospitalized about 10 times for asthma. Once, she spent two weeks in a hospital bed, taking oxygen every two hours along with medicine to relax the constricted passages to her lungs, her mother said.
"I was afraid she was going to die," Contreras recently recalled.
Families who live in Contreras' ZIP code on the west side of Salt Lake City, 84116, experience that sickening fear more often than parents living almost anywhere else in Utah, according to an analysis of Utah Department of Health data requested by The Salt Lake Tribune.
The rates of children seeking care in an emergency room and being hospitalized for asthma are higher in certain Salt Lake County ZIP codes — mainly west of Interstate 15.
The rate of children under age 4 seeking emergency room care who live in the southwest part of Salt Lake City, including Glendale and Poplar Grove, is three times higher than the state average. The rate is up to 10 times higher than in parts of Orem.
The hospitalization rate of children living in Tooele County, the west side of West Valley City and the northwest part of Salt Lake City, including Rose Park, is about two times higher than the rest of the state. The rate is eight times higher than in Cedar City.
Contreras still doesn't know what triggered her daughter's attacks, she said in Spanish. She's just hoping the now 10-year-old will grow out of the lung disease.
Utah public health officials are also in the dark about why asthmatic children in some neighborhoods struggle to breathe more than others. Unlike officials in states like California and Michigan, Utah doesn't look at disparities by race, ethnicity or income levels among people who check into hospitals.
The reasons families head to the ER can be complex: Some children's asthma is more severe; they may have other health problems; triggers like cold weather and respiratory infections may not be easily avoided; parents may not know their child has asthma until after the first ER trip. But the visits often are linked to a family's income, education and neighborhood location, according to national research.
Some Utah areas with high hospitalization rates have higher concentrations of poorer and less educated families. Low education levels are tied to higher levels of smoking — and secondhand smoke worsens asthma symptoms in children.
Children in low-income families are more likely to live in substandard housing, which is tied to exposure to triggers such as cockroaches and mold. Also, they are less likely to have access to primary care or asthma medications.
Neighborhood placement matters, too: Research shows asthma is worse for children who live or attend school near freeways because it exposes them to higher doses of pollution than surrounding areas receive.
"It might be very difficult for someone in a lower [socioeconomic status] to miss work to take a child to a provider, even if they have one," said Bryan Stone, a doctor at Primary Children's Medical Center after seeing the Tribune data, explaining generally why income matters to health.
"Just the placement of I-15 on the west side of the valley, the lack of mass transit and more automobiles — there are all sorts of things that are known risk factors for asthma hospitalizations that can play into this," he continued.
While it's not clear that those factors are the cause of Utah's disparities, some public health officials are starting to tackle smoking, home environments and freeways to help children most at risk.
—
To read stories about these efforts, click on the links at the top left-hand side of the page
—
This story was reported with the assistance of interpreter Maritza McKee. —
What happens during an asthma attack
People with asthma have oversensitive lungs and airways. During an attack, the airways become inflamed and filled with mucus, and the muscles surrounding the airways constrict in response to triggers such as pollen, pollution, stress, cold air or physical activity. It's like sucking air through a straw, Intermountain Healthcare says. During an asthma attack, breath often whistles as it moves through the restricted airways. For relief, sufferers need medications to relax the airway muscles. Asthma's burden, by the numbers
Among Utah adults, 8 percent, or 155,000, have asthma.
Of these …
12 percent said they lost sleep on five or more days during the past month because of asthma symptoms.
18 percent experienced asthma symptoms every day during the past month.
12 percent visited an emergency room or an urgent care center for asthma within the past year.
21 percent visited their doctor for urgent treatment within the past year.
689 were hospitalized for asthma in 2008.
Among Utah children age 17 and younger, 7.3 percent, or 63,000, have asthma.
Of these …
34 percent of school-age children missed at least one day of school during the past year because of asthma symptoms.
20.5 percent of middle school and 17 percent of high school students said they experienced activity limitations at least one time per week because of symptoms.
64 percent experienced an asthma attack during the past year.
16 percent visited the emergency room or an urgent care center for asthma, and 30 percent visited a doctor for urgent treatment in the past year.
741 were hospitalized for asthma and 2,400 were treated and released for asthma in 2008.
Sources: "Asthma in Utah Burden Report 2009," Utah Department of Health "Asthma FastStats." —
About the project
This article was conceived and produced as a project for The California Endowment Health Journalism Fellowships, a program of the University of Southern California's Annenberg School for Communication & Journalism. —
Monday: Reducing hospital visits
P Primary Children's aims to slow the revolving door of asthma hospitalizations through education, and an Orem mother blogs about asthma-proofing her home.