This is an archived article that was published on sltrib.com in 2012, and information in the article may be outdated. It is provided only for personal research purposes and may not be reprinted.
Ogden • By the time Camilla Black Grondahl became pregnant with her second child in 2010, she had already watched two older sisters bury sons who were born with a congenital affliction that gave them the appearance of "little old men." Various health problems made their survival impossible.
The young mother did not know whether she, too, could pass the condition to her unborn son. But a Utah researcher, who had been sequencing her family's genes, did know.
Gholson Lyon's research team had detected a mutation in her genome that gave any boy she conceived a 50-50 chance of sharing the heartbreaking fate of his cousins and uncles.
"My jaw dropped open. Who would have thought that another mother would get pregnant during this research and it would be a boy?" said Lyon, then a professor of psychiatry leading the University of Utah's genetic research into the disease.
He found himself in an ethical quandary that is bound to become more common in biomedical research. As technology advances and costs come down, gene sequencing is becoming routine — yet no system is in place to alert study volunteers about results that could have crucial bearing on their health.
Lyon is a physician, but he was not comfortable with warning the Grondahl family. He was not Camilla Grondahl's doctor. And the gene sequencing, like almost all testing done for biomedical research, was not done in a clinically certified manner.
What if the data were wrong and the young woman terminated her pregnancy?
Nor was he comfortable not sharing the results with the family, who had welcomed him into their home.
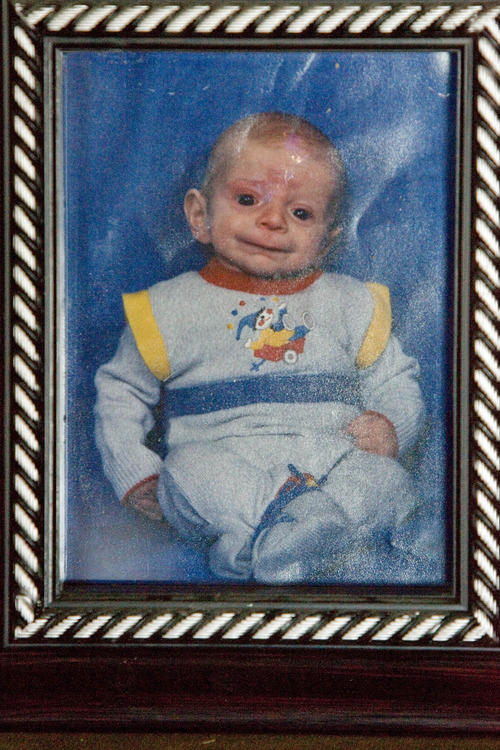
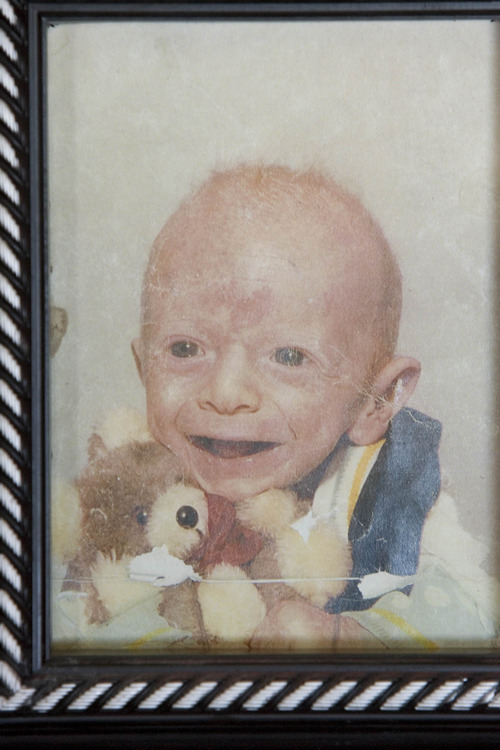
Last February, the Grondahls' son Max was born with the telltale signs of the then-unknown disease: wrinkled skin, hernias and facial deformities. By the time "our valiant hero," as his parents called Max, died four months later, U. researchers had a name for the disease: Ogden Syndrome.
In a commentary published this week in the top-shelf science journal Nature, Lyon describes the ethical dilemma that he and other genetic researchers face when they find genes with medical consequences for those they are studying.
"At the moment, human-genetics researchers operate in a totally unregulated environment, following their own protocols to obtain, store, track and analyze DNA — creating many opportunities for error," Lyon wrote. "But when the result can mean the difference between life and death, mistakes are not an option."
He proposes requiring that all sequencing of human genes follow strict federal guidelines known as Clinical Laboratory Improvement Amendments, or CLIA. The move would add physicians to each study, who would order certified testing and ensure volunteers received genetic counseling to explain the results.
"In this way, when participants want to know what we know, we will feel confident that what we tell them is correct," wrote Lyon, now a research scientist at the Children's Hospital of Philadelphia. Next month, he is moving to Cold Spring Harbor Laboratory, a leading genetics research institution on Long Island.
But Lyon concedes there are no simple answers, although he believes his proposal could save society money in the long run since the resulting information could prevent disease in some cases and improve treatment outcomes in others. And sequencing DNA in centralized certified-facilities could be less costly, thanks to economies of scale, and avoid unnecessary duplication of sequencing.
But if all laboratories that might make discoveries related to volunteers' health were required to be CLIA-certified, research costs could be driven up, said Lynn Jorde, the chairman of the U.'s human genetics department and the past president of the American Society of Human Genetics.
"It would cost a great deal of extra money," Jorde said, "at a time when research funding is rapidly vanishing."
—
A genetic detective story • Jorde is one of the many U. co-authors on Lyon's study that identified Ogden Syndrome, named for the Utah city where Halena and Gary Black have lived as two infant sons and three infant grandsons have succumbed to the same strange failure to develop.
The scientific detective story begins in 1979, when the Blacks' son, Kenny Rae, was born with sunken eyes, eczema, and other signs that would become painfully familiar.
A second son, Hyrum, was born in 1987 with the same appearance. At the time, Halena did not suspect the boys' similar features were linked to their failure to thrive. They were brothers; why shouldn't they look alike?
But their autopsies drew the attention of U. pediatrician John Opitz, then working at Primary Children's Medical Center, on his way to becoming a leading medical geneticist.
Halena hails from a large Mormon family. Her parents had 58 grandchildren, but only her two boys had the disease. Her sisters gave birth to healthy boys. Halena gave birth to a stillborn girl, but her five other children — four daughters and a son — remain healthy.
Then her daughter Sesha gave birth to her own "little old man," as the family calls the children, in 2007 in St. George. This boy, named Corbin, failed to develop normally. When his scrotum turned purple, commonly caused by a hernia, Halena suspected he would die from the same condition that killed her sons.
Two years later, her daughter Kimberly VanderDoes gave birth to a second son, Sutter. While the older boy was healthy, Sutter had Corbin's symptoms. Both boys died at Primary Children's — Corbin at 5 months and Sutter at 15 months.
Recalling the Black boys two decades earlier, Opitz examined Corbin's autopsy report, then told Halena he strongly suspected a genetic disease was at play, one that had never before been described.
"He said, 'I am not going to brush this under the rug. We're going to get to the bottom of this,' " Halena said.
Around then, Lyon, who has a doctorate in chemical biology, joined the Utah faculty to investigate the genetic basis for psychiatric disorders. Colleagues introduced him to the Blacks, and a research project was launched.
Lyon visited the extended Black family in Halena's living room in 2009 during a pre-Thanksgiving gathering. He brought a student who helped him draw blood samples from several of the adults, including Camilla and her youngest sister Eliza, for genetic testing.
—
Genetic research hot spot • The family illustrates why Utah attracts genetics research. Families tend to be large, remain geographically close and keep track of their pedigrees, which can help scientists track the relationships between genes and diseases.
Using a new algorithm developed by U. researchers, Lyon's team scoured parts of the genomes of Halena and her daughters for a gene that could be responsible for the boys' condition. It was like searching for "a needle in a haystack," Lyon later wrote, but the team pinpointed the mutation. By then, Camilla had become pregnant, and the family shared the news with Lyon. Concerned for Camilla, they asked Lyon what he knew.
The data suggested Camilla carried the gene, but Lyon was unwilling to reveal the results because he could not be certain of their validity. For this same reason, he cannot divulge which way the data points for Eliza, who plans to marry this year.
"He said he couldn't tell me. With [Camilla] being pregnant he didn't want her to have undue stress," Black said. "It was a smart move on his part to keep it under the belt."
But Lyon remains troubled. He has started a nonprofit, the Utah Foundation for Biomedical Research, but wonders whether he wants to continue sequencing human genes until his ethical concerns are resolved by the larger research community.
A more recent dilemma arose as he investigated genetic foundations for attention deficit-hyperactivity disorder. He had sequenced genetic samples provided by a father and two sons with severe ADHD, but in an unrelated finding, he pinpointed the genes responsible for one of the son's anemia.
"But I was not able to return any results to him, because this research was not performed in a clinical environment," Lyon wrote. "Wouldn't it help him to know that the jaundice and other problems he had battled for the past 20-plus years of his life were caused by two rare recessive mutations?"
—
Moral obligations • Opitz, renowned for identifying several genetic syndromes, agrees that research needs new rules. He is grappling with the same issue as he studies a family in which some boys are born with a devastating mineral imbalance. Opitz's data indicate a family member carries the culprit gene, which could be passed down.
"These are not uncommon occurrences, but there is no way to predict them when you start this kind of research," Opitz said. "Some [researchers] seem to think that these findings can be shared in print with colleagues in the hope that the data is so anonymous that the family has to do hard work to figure out what it means. I don't like to be in that position. I like to be open and above board."
According to U. law professor Teneille Brown, this quandary will become more common as researchers increasingly stumble upon "medically actionable" results in genetic testing.
"There is a moral obligation to return those results [to volunteers]," said Brown, an expert in biomedical ethics. "They don't see themselves being in these discrete categories of research subjects or patients. They want to be seen as patients."
But disclosure could create new questions. What if a person has no wish to learn that his genes put him at risk of Huntington's disease, or some other devastating condition unrelated to the research he volunteered to help?
Then there are legal issues.
"What do you do with a researcher who is a physician? Can you sue them for malpractice even if they are wearing their researcher's hat?" Brown asked.
—
The gift of closure • Halena Black feels U. researchers treated her family compassionately. She is grateful that she now knows why her sons and grandsons died and feels honored to be part of the research.
She is publicly sharing her family's genetic secret to help others who may have lost sons to the same mysterious disease. So far, a California family that lost three boys has been identified as carriers, thanks to the U. research.
"She is an extraordinarily courageous and wonderful lady," Opitz said. "She was extremely realistic when it sunk in that each of her daughters might be a carrier. Once the boys were buried, she was willing to get on with life in a realistic manner and say, 'What do we do next?' "
The Blacks' newest grandson, Max, was born on Feb. 2, 2011.
"We didn't know Max had it when he was born a month early. He was swollen up. It took about a week," Halena said. "It hit Camilla the very worst because she had lived through her brother [Hyrum], and through her nephews. She knew what the outcome was going to be and accepted it."
The Grondahls did not take extraordinary measures to extend the boy's life, preferring to make him comfortable at home and allow him to die in peace with his family. He passed away at four months, in Halena's living room on Father's Day last year.
The youngest of the Black daughters, 22-year-old Eliza, is engaged to marry in September and hopes to have children. Lyon has encouraged her to get an official test, which recently became available at ARUP Laboratories.
"I would like to know, but at the same time, I'm nervous to find out," said Eliza, who intends to get the test. "I'm scared. I don't want to go through what my sisters went through."
Camilla said she would like to have another child, but isn't sure she could handle the stress if she became pregnant with a boy who might never grow up. She said she could instead use in vitro fertilization, which would allow doctors to identify and implant a healthy embryo.
"Otherwise it's a 50-50 chance, a coin flip," she said as her 2-year-old daughter, Chloe, spread photos of her late brother on the floor. No one knows whether the little girl carries the Ogden gene.
Mothers and sons: Odgen Syndrome
University of Utah researchers identified this rare congenital disease last year, linking it to a genetic mutation that is passed down the mother's line. Girls don't acquire the disease, but boys are born with severe health problems and facial deformities that give them an aged appearance. Five baby boys born to an extended Ogden family succumbed to the disease.
Kenny Rae Black, b. 1979
Hyrum Black, b. 1987
Corbin Lundell, b. 2007
Sutter VanderDoes, b. 2009
Max Grondahl b. 2011