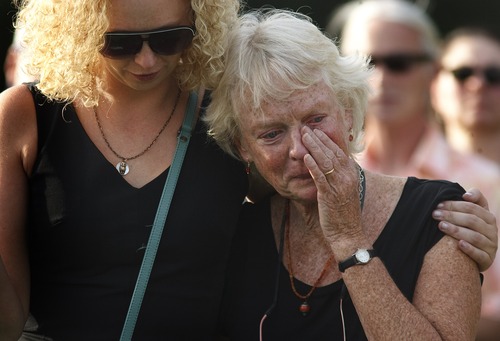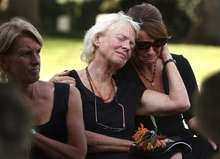This is an archived article that was published on sltrib.com in 2013, and information in the article may be outdated. It is provided only for personal research purposes and may not be reprinted.
On a Thursday morning in late July, Sara Battin Pearson got an unexpected phone call from Brooke Hopkins, who jumped right to the point: "I want to die, Sara."
It was the first time Sara had heard her 71-year-old stepdad express so emphatically his desire to be done with this life. Sure, Brooke, a beloved University of Utah emeritus English professor who was paralyzed in a 2008 bike collision, had said before that his pain was unbearable or that he doubted he would live through the night. But this time his words were less descriptive, more decisive — like a demand or an impassioned plea.
On the other hand, Mike Battin, Sara's brother, had heard Hopkins say many times in the years after the accident that he wanted to die, but his request had grown increasingly urgent in recent months.
Students who took Brooke's spring class on Moby-Dick were aware that he probably wouldn't be around to teach Don Quixote in the fall. His in-home caregivers knew he was yearning for release.
And 72-year-old Margaret Pabst Battin — known as "Peggy" — Brooke's wife of 27 years and a nationally renowned medical ethicist who specializes in end-of-life issues, had had numerous conversations with her husband about dying over the decades, but especially in the past year.
Often, though, he was ambivalent, Peggy felt, seesawing between desiring death and loving life.
When family members gathered July 31 at the couple's Salt Lake City Avenues home to say their final goodbyes, hospice workers asked for an hour's delay to get the appropriate pain medication. Peggy, wishing, perhaps, to hold on to him a little longer, suggested maybe they should come back "tomorrow."
Brooke retorted, in his deep, hoarse voice, filled with frustration: "I don't want there to be a tomorrow."
—
A patient's right • Conversations about when and how to die are much more common in families these days than they were even a few decades ago.
When life-supporting technologies such as ventilators were introduced, the thinking among many was that once such equipment was attached, it would be immoral or unethical to discontinue their use — even if the patient didn't want to go on.
Slowly, through discussion, disagreement and debate, that worry has been replaced by an emphasis on a patient's right to choose whether to continue such life support.
Several generations of doctors now have "grown up with the understanding that the physician's sole obligation is not to prolong life at all costs but to abide by a patient's wishes," says Alan Meisel, a leading authority on end-of-life decision-making and founder and director of the University of Pittsburgh's Center for Bioethics and Health Law.
There is now a "national consensus on end-of-life care," Meisel says, "that it is permissible both legally and morally — and as a practical matter — to terminate life-sustaining treatment when patients no longer want it or when they left instructions [beforehand] that they wouldn't want it."
Even many religious guidelines do not oppose withdrawing such life-sustaining treatments.
"Discontinuing medical procedures that are burdensome, dangerous, extraordinary or disproportionate to the expected outcome can be legitimate; it is the refusal of 'overzealous' treatment," the Catholic Catechism says. "Here one does not will to cause death; one's inability to impede it is merely accepted."
In Utah, the Advance Health Care Directive Act, enacted in 2008, recognized that "developments in health-care technology allow the unnatural prolongation of life," explains Leslie Francis, a University of Utah law and philosophy professor who writes about advance directives, disabilities and access to medical care.
The law states that competent patients "should have the clear legal choice to accept or reject health care," Francis says, quoting the statute's wording, "even if rejecting health care will result in death sooner than death would be expected to occur if rejected health care were started or continued."
It is important, she says, not to create conditions in which people are afraid to start a treatment for fear they can't stop it later. "You don't want a world in which you can't try and see what kind of outcomes you can get."
When patients conclude that they are done trying, hospice doctors and nurses can help family and friends respect the patients' wishes.
"We want to make them comfortable, to allow them to let go," says Carla Prepejchal, a Utah hospice nurse and case manager who was not involved in Brooke's care but has tended to many dying patients. "We give medication to deal with any symptoms they may have — it could be agitation, air hunger, lashing out, vomiting, bleeding. But we don't do anything to hasten someone's death."
The goal is "to control the symptoms," Prepejchal says, "so patients have the highest dignity before they die."
That's the aim of Utah's law, too, to permit patients to "die with a maximum of dignity and function and a minimum of pain" — in short, exactly what Brooke was seeking.
—
An exuberant life • Brooke and Peggy arrived at the U. the same year, 1975. He was fresh from Harvard with a background in 18th- and 19th-century British literature. She had a master's degree in writing and a doctorate in philosophy from the University of California at Irvine.
He was a tall, handsome, lanky outdoor enthusiast, gourmet cook and a lively conversationalist. She was a fair-haired beauty and rigorous thinker, questioning every assumption, always arguing the opposing points of view.
Sparks flew from the start, and within a year, they moved in together. Seven-year-old Sara, Peggy's daughter from a previous marriage, came to live with them. Her son, Mike, 2 ½ years older than Sara, visited on holidays and summers. The couple shared an action-packed academic life, traveled to exotic locales, danced all night in undiscovered backwoods blues joints and tasted a rich variety of spicy dishes and good wine.
They married in 1986.
Brooke became one of the U.'s most popular professors as he explored the works of Romantic poets and the genre of autobiography.
Peggy emerged as a pioneer in the field of bioethics, specializing in end-of-life questions. Suicide. Euthanasia. Do Not Resuscitate orders. When and how to die. She cranked out essays, compiled collections and edited volumes on death and medicine. Soon she was known for titles such as The Least Worst Death and, more recently, Ending Life: Ethics and the Way We Die.
Yet it was always about other cases, other people, other circumstances.
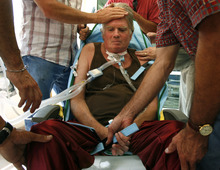
That is, until Nov. 14, 2008, when her husband, biking down City Creek Canyon, collided with another rider and broke his neck. Brooke became a quadriplegic, paralyzed from the shoulders down.
Many people with spinal-cord injuries say they want to die when they first learn the extent of their injuries and the challenges ahead. Research shows that if they make it through that initial year, most are ready to embrace life as it is.
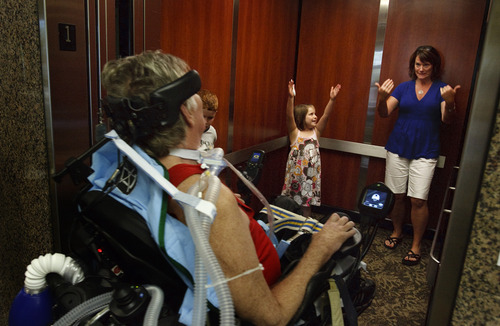
That was clearly the case with Brooke, who developed a fierce desire to fight on, seeing his limitations as an "adventure."
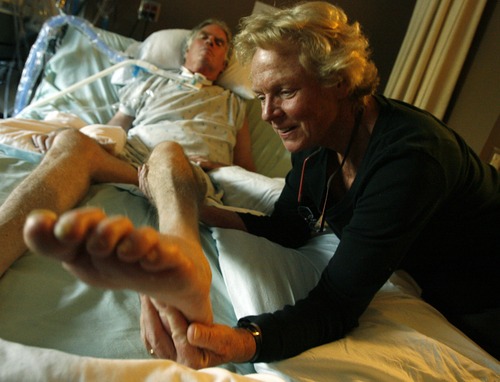
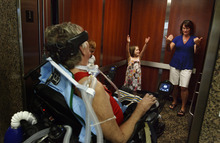
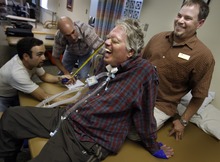
He labored diligently to breathe on his own and regain small movements in a few fingers and toes. He learned to navigate his wheelchair with his head and then with fingers on his left hand. He could write emails using voice-recognition technology and taught courses to retirees — many of them fellow educators — in his living room. Thoreau's Walden, The Iliad, The Odyssey, The Aeneid, Dante's Divine Comedy, The Canterbury Tales, Shakespeare's sonnets and "The Tempest."
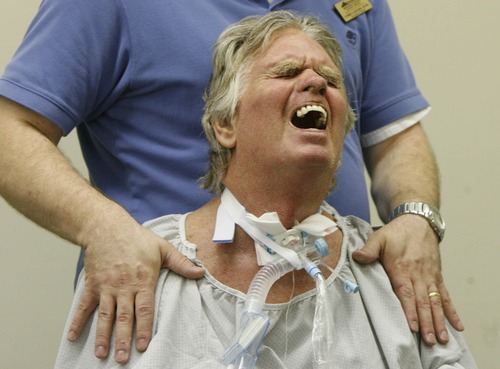
But setback after setback — infections, pneumonia, spasms, sleeplessness, repeated hospitalizations — led to a slow, steady decline in the past year or so. He finally had to give up one of his great pleasures, eating, and be fed through a tube.
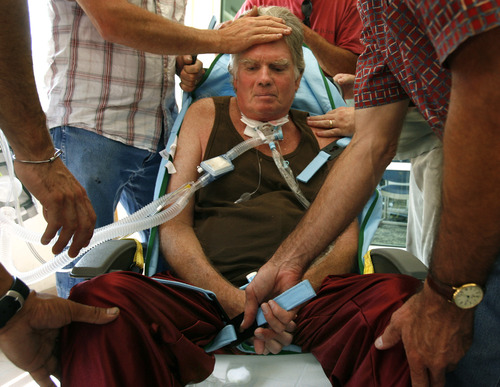
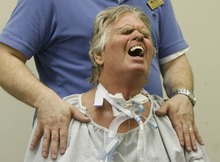
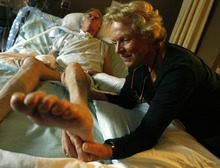
A person of great dignity, Brooke suffered daily, almost hourly indignities, from suppositories every morning and constant suctioning to being rolled over, poked and prodded, bathed and bothered.
Last summer, Brooke had had enough and wrote what he called his "final letter" to family and friends.
"Relentless pain corrodes the soul. Mine has been corroded to the point at which I simply no longer desire to live in this condition. … Is this selfish on my part? Maybe. If it is, I am deeply sorry. I am especially sorry for what it will do to Peggy, who has done so much to keep me going," he wrote. " … [Peggy's and my] life together has been an incredible adventure. Oh, my God, what an adventure. Even after the accident. But the time has come."
He never sent the letter.
Brooke rallied enough to direct two more courses on Moby-Dick in fall 2012 and spring 2013 but required extensive assistance from an English professor colleague. He no longer could talk much or lead discussions. Though students treasured his presence, he could make only occasional comments.
In recent months, Brooke couldn't "hold much of a conversation with us," Sara Pearson says. "He wasn't able to be as present."
Pain comes "in many forms, not just physical," she says. "His face was etched in pain all the time."
Dave Mickelsen, a longtime friend, also saw the decline.
"Brooke's interest in and ability to interact with other people — which had been his hallmark — were contracting," Mickelsen says. "The horizon of his interests was radically reduced."
The last class met in the couple's home July 15.
Brooke then turned to a new goal: dying.
"In the past there had been dramatic moments in which Brooke would say he was in agony," Mickelsen recalls. "Now there were no histrionics. It was more matter-of-fact, a conscious, reasoned decision."
But how to do it?
—
The last day • When Mike Battin walked into the Avenues home on Saturday, July 27, Brooke's first words were not "hello" or "how are you?" but rather, "I want to terminate my life."
On Sunday, when Mike's sister, Sara, arrived, his message was the same.
"I am dying," Brooke told her. "I want to be free."
Both children saw their role as listening and being supportive, while helping their mom accept his wishes. The talk was only about how — not whether — this was going to happen.
On Monday, the family went with Brooke to see his primary physician so the doctor could hear for himself Brooke's decision and mental competence.
The retired professor told him, "I'm alive and I'm dead," Mike recalls, and the family at first had a tough time deciphering what he meant.
"I think what he was trying to say was that although he was alive," Mike says, "it was only because of the machines."
In other words, he would be dead without them.
Peggy wanted to ensure that there wasn't some kind of physical problem that was prompting his desire to die — an infection, for instance. She asked for more blood tests to rule it out. They all came back clean.
By Tuesday, the doctor recognized and respected Brooke's resolve — and referred the family to hospice.
The next morning, the family met with a hospice doctor.
"She had the best bedside manner of any physician I have ever met," says Mike, a former EMT who has dealt with hundreds of doctors. "She told us in her 11 years with hospice, she had never seen anyone so convinced, so resolute as Brooke."
Together, they worked out a plan for his passing — that very day.
Brooke would receive medication for anxiety and pain. His life-sustaining machines — including a ventilator and a diaphragmatic pacer, which helped regulate his breathing — would be scaled back.
Neither external oxygen nor his feeding tube was in use, and his cardiac pacer did not require turning off.
In the past, when respirators were removed, many patients suffered from air hunger, which left them gasping for breath, the hospice doctor told them. Medications now can block those impulses, but are not the cause of death.
That knowledge gave Brooke the assurance that it would be a gentle way to go.
"We all had the same message — this is a good thing, let it happen," Mike Battin says. "There was not a wavering moment in any of us."
Except in Peggy.
Though she agreed intellectually with the decision, she was not ready. She wanted more time.
And, yes, despite her bedrock conviction that a person should have the right to be the architect of his or her own death, it was emotionally devastating.
"You can't imagine anything more intensely personal, because I love this person," she had said in 2009, her voice cracking, tears in her eyes at the prospect of his death. "But there are two components to love — love is partly wanting to be with him, but it's also wanting what's best for him and wanting to want what he wants. What he wants and needs might be different from my self-interests."
No one else would feel the loss as deeply as Peggy, the one who had been his companion and lover for decades, the one who had cared for him in his last years of agony and transcendence, the optimist who saw the possibility of more good days ahead.
Now his death was imminent, Peggy knew. Wednesday. Today.
But wait, the hospice workers said they needed an hour. Instead of scheduling his passing to begin at 1:30 p.m., it was pushed back to 3.
How to fill the time?
Brooke called a number of his close friends to say goodbye. He had already written his epitaph, picked out a Salt Lake City Cemetery plot, settled on burial rather than cremation. But he hadn't selected a headstone. So the almost-gleeful professor in his wheelchair led a tiny band of family, friends and caregivers — in what was dubbed the "Hopkins Liberation March" — a few blocks to the Salt Lake Monument Co., next to the cemetery. They found just the right one and returned to the house in the sweltering July heat, Peggy and Sara stopping for an ice cream cone along the way.
At around 3 p.m., the hospice doctor gave Brooke drugs for anxiety. The end had begun.
"Thank you" were his last words to Mike. To Peggy, "I love you."
Brooke was getting sleepy, so they moved him to his bed. The necessary machines were slowly turned down. Peggy curled up next to her husband for the last time. A CD of Marion Williams' "My Soul Looks Back" played quietly as he drifted away.
"It was peaceful and painless," Peggy says, "just as he wanted it."
It was, indeed, a least worst death.
Brooke died "of his injuries from the accident, which became an inevitable downhill course," says Francis, the legal expert and family friend. "Doctors intervened and intervened and intervened to reverse that course, but he eventually reached a point where their interventions were no longer acceptable to him."
A small army of friends gathered two days later at the cemetery to remember Brooke, to praise him, to place flowers on his casket.
"Brooke showed a lot of dignity, great grace and spirit, and strength under the worst of circumstances," says his sister, Lisa Hopkins Wheeler, who came from New York City for the occasion. "He expressed all of that in his decision finally to end his life."
A friend at the service mentioned he once asked Brooke about a set of narrow, wooden skis hanging on the wall. The intrepid English professor said he had used them to ski the Wasatch Mountains' "Little Matterhorn," a popular yet arduous backcountry destination.
Brooke wasn't a great skier, another friend acknowledged, but he was unafraid of plowing down a scary mountain or jumping into the unknown — including death.
And what of Peggy and her views about the end of life?
She still supports a person's right to choose, she says, but "autonomy is way more complex than you ever could have imagined — and this is true not just for Brooke but for every person who faces the end."
You can't assume that "all choices are alike," she says, "so you have to be alert to what someone deeply wants."
She believes "in honoring a loved one's wishes," she says, her voice dropping, "even if it is painful to you."
And, she adds, it is.
Facebook: peggy_fletcherstack
Twitter: @religiongal —
Past stories
Read more in The Salt Lake Tribune's series about Brooke Hopkins:
Tragic metamorphosis: Ethical debates turn personal for U. professor
Learning to live again: Brooke Hopkins struggles through rehab after bicycling accident
Long-awaited homecoming for paralyzed U. professor
Utah professor's odyssey brings him home to new joys, new pain
For disabled Utah professor, there's no place like home
Learning to live again: How a new device may help Brooke breathe —
Brooke's 'final letter'
Dear family, friends, and caregivers,
First, I want to tell you how grateful I am for the love and support you have given me over the past almost four years since my accident in November of 2008. Without that, I would never have survived as long as I have. I'm immensely grateful for this and I hope that I have repaid it in some measure by my own willingness to go on despite considerable odds. I wish I had the words to tell you how much you have meant to me, but I simply don't.
But now I want to tell you that I've decided that I can no longer go on living in a situation that I have been in over the past five months since my pneumonia. A great deal of this has to do with the relentless pain that I have suffered over those months. I have struggled with this, needless to say. On the one hand, I want to keep on fighting and above all to keep on teaching. On the other, I find that I've reached the limit of my capacity to go on. It is simply just too hard. Pain eats away at your soul. For many years since the accident, I have been motivated by a deep will to live and to contribute to the benefit of others in my small way. I think I have done that. And I am proud of it. But, as I have told [my wife] Peggy over the past few months, I knew that I would reach a limit to what I could do. And I have arrived at the limit over the past couple of weeks. I knew that there would come a time when I would reach that limit. I didn't know when it would be. But I knew that it would come, and it is here, now. You may think that I'm depressed. I am. And I have every reason to be, I think. But that doesn't take away from the fact of what I am currently feeling. Despair. And hopelessness.
I don't mean to come across as self-pitying. I am not. I am simply at the end of the line and what I can tolerate. As I've said, relentless pain corrodes the soul. Mine has been corroded to the point at which I simply no longer desire to live in this condition. I do not know how I will go about departing. It's very complex. I do not have a terminal condition. In fact, because of my diaphragmatic pacer, I could go on living for a very long time (unless of course I come down with another bout of pneumonia, which is probably inevitable anyway). But I do know now that I do not wish to continue to live. Is this selfish on my part? Maybe. If it is, I am deeply sorry. I am especially sorry for what it will do to Peggy, who has done so much to keep me going. To keep me motivated. (Believe me, I am crying as I write this.) I have pulled in many different and contradictory directions. On the one hand, part of me wants to keep on fighting. On the other, I simply wish to give up at this point. As I say, I have no idea how I will arrange for my own departure from the beautiful life I have lived. Peggy and I have had an amazing 35 or so years together. There have been some rough moments as there are in any deep relationship as long as ours. But our life together has been an incredible adventure. Oh, my God, what an adventure. Even after the accident. But the time has come. I think she understands this. I do not wish to bring her any more grief and sadness about my condition. And my state of mind as it has evolved over the past few months. But the time has come.
Forgive me. You have all been so loving and generous. Thank you.
All my love, Brooke
(Dated July 28, 2012, about a year before his death) —
More photos, videos, stories
To see more photographs, view videos and read previous stories about Brooke Hopkins' ordeal, go to http://www.sltrib.com.