This is an archived article that was published on sltrib.com in 2013, and information in the article may be outdated. It is provided only for personal research purposes and may not be reprinted.
Murray • In the hospital room of the future, a patient stay won't include being poked and prodded for vital signs every few hours by a nurse, or loud beeping monitor alarms that sound with every wiggle in bed.
Patients will be able to talk with doctors remotely by computer so that changes to care can be made almost in real time, not just once every 24 hours when physicians make their rounds. They'll use tablets to order meals from the kitchen, movies from Netflix or to call a nurse.
And, thanks to technology and the innovative work of Intermountain Healthcare's new Transformation lab, the future may not be so far away.
The 20,000-square-foot Murray lab was founded by Intermountain and technology companies Xi3 and Intel. It's work also includes collaborations with tech companies Dell, NetApp, and Sotera Wireless.
Their shared goal: Leverage technology to improve the patient experience and deliver better care more efficiently.
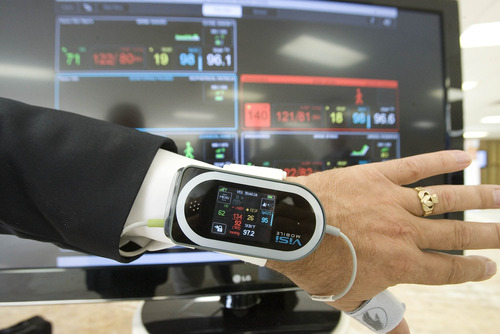
In practice that might translate into using wireless monitors to track patients' vital signs remotely from the nurses station, or changing the brightness or color of the lighting in hospital rooms. Lighting can replicate circadian rhythms so patients can rest, or be used to create settings that are more conducive to better care; pink lighting, for example, has a soothing effect on kids with autism, making it easier to treat them.
"It's all aimed at health care, and it's all aimed our mission and our desire to be a model in health care for [Utah] obviously, to the nation and the world," said Fred Holston, Intermountain's chief technology officer.
It could also prove profitable if the technologies or products developed are ultimately sold commercially. Intermountain partner Xi3, for example, is using the lab as a testing ground for the company's cube-shaped modular computers and micro-servers, which control the technology in the re-imagined patient rooms. Later, the partners plan to market the technology to other health care providers.
The use of technology isn't new to medicine or to Intermountain, but it wasn't until about three years ago, that the tech staff started tinkering with turning homegrown ideas into staff-built products and software or partnerships. Success wrought credibility and over time earned the tinkerers a bigger space and eventually the lab, Holston said.
To date the team has designed and built a variety of patient safety tools, including a heartbeat monitor that sounds an alert for patients at risk of suicide and an electronic sensor that reminds caregivers to raise the side rail on a crib to ensure the littlest patients stay safely inside. Other lab-driven projects have simplified patient-data collection, like a mobile application used by medical helicopter teams for recording vital signs and other patient details. In the past, the information was recorded twice, first on paper and then in the computer. Now it can be uploaded from a tablet to a database, saving time, lab manager Billy Prows said.
Another innovation: A prototype watch that reminds nurses to wash their hands before and after each patient interaction. A sensor triggers a glowing red light on the watch when the nurse walks through the door. The light goes green after contact with water and then glows red again when the nurse leaves the room.
"This is designed to be very low cost and just a reminder like a seat belt light, because our caregivers today are more busy than ever," said Prows. The hope is that the reminder will increase hand washing and reduce the rate of hospital-acquired infections, which can increase the time a patient stays hospitalized. That could result in significant savings, since insurance won't cover the cost of treating those diseases, Prows said.
The lab hopes to get the prototype watch in a pilot study at Intermountain hospitals soon, he said.
Twitter: @jenniferdobner