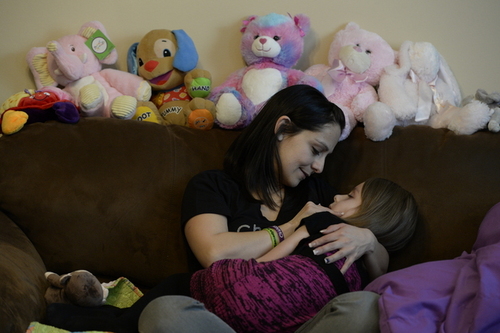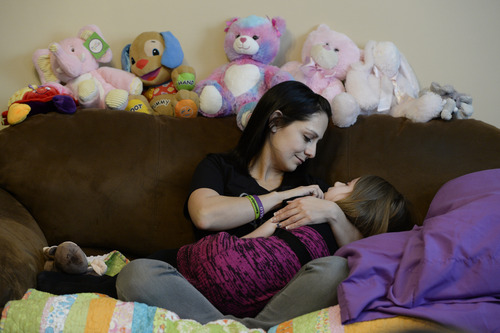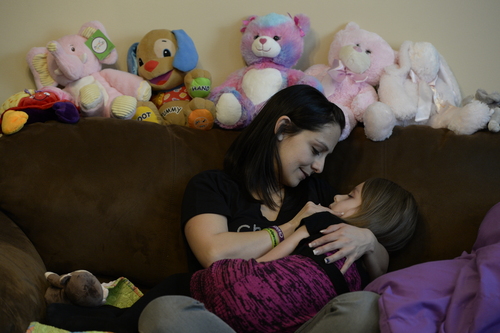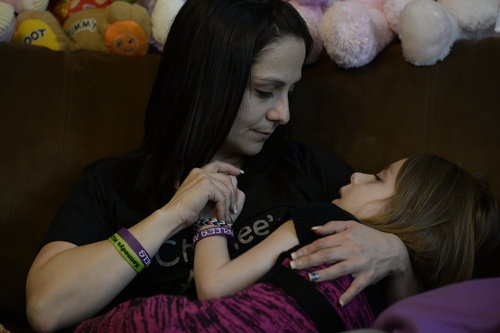This is an archived article that was published on sltrib.com in 2014, and information in the article may be outdated. It is provided only for personal research purposes and may not be reprinted.
West Jordan • No longer needed, an oxygen tank sits idle on the living room floor. Nearby is a box of purple bracelets that Charlee Nelson's family made to raise awareness of Batten Disease and to collect donations to cover the 6-year-old's medical costs.
Across the room, hanging from the stroller Catrina and Jeff Nelson had to buy for their once active, gregarious child is a burial dress.
"My [oldest] daughter was recently baptized and we were shopping for her when I saw this and thought, 'This is the dress we have to get [for Charlee]. It's the wedding dress she'll never get to wear,' " Catrina said, fingering the white, satin gown.
Three years ago Charlee Nelson was singing the ABCs and waving to strangers on grocery store outings with her mom. Family movies show her fearlessly plunging into the swimming pool, dancing with her older brother and sister and making silly faces for the camera.
Today she is blind, bedridden and near death.
"She's hanging on, but she's not doing too well," Catrina says, cradling her nearly lifeless "baby" girl on the living room couch.
Charlee is among 50 Utah children on a waiting list for a nonintoxicating cannabis oil shown to quell seizures in children with untreatable epilepsy. Utah lawmakers are debating a bill, HB105, that would allow families to import the oil from Colorado where marijuana is legal and the "hemp supplement" is produced.
The bill rests in the Senate and from there needs only Gov. Gary Herbert's signature before becoming law.
But Senate leaders are considering placing more restrictions on the bill that could impede access to the oil, families say. "We're working through their concerns," said an optimistic Jennifer May, the mother of a boy with Dravet syndrome and founder of the grass-roots group, Hope 4 Children with Epilepsy.
Whatever legislative fix lawmakers settle on will come too late for Charlee.
"We would have loved to try [the oil]," Catrina said. "But I'm still hopeful it will give these other kids a more normal life, that it will take away the pain and seizing and let them sing, dance and ride bikes again."
Charlee has Batten disease, a rare neurological disorder occurring in fewer than four of 100,000 births in the United States.
She lacks an enzyme needed to remove fatty waste from the cells of her brain, eyes, skin and muscles. The accumulating waste leads to seizures, mental impairment, blindness, loss of bodily control and eventually death — a fate cannabis oil can't change.
There is no cure, said Catrina, who nevertheless wonders whether the oil might have kept the brain-damaging seizures at bay, prolonging and improving her daughter's quality of life. "We lost a lot of time diagnosing and treating her atonic seizures. Time is what it might have bought us. That's what it kind of boils down to, time."
Charlee's first seizure was in May 2011.
Nelson and her husband, Jeff, had flown to Colorado for a [niece's] graduation. They had just landed and were grabbing lunch at Popeye's when Nelson's sister-in-law called to say Charlee had a seizure and had been taken to the hospital by ambulance.
"We just looked at each other and both of us started to sob," Catrina recalled.
Doctors initially thought it was an isolated event but scheduled testing a week later to be sure.
While waiting in her hospital room, Charlee froze and stared at the wall, then fell to the ground. "That was the first seizure I had seen. I broke down and thought, 'This isn't happening,' " Catrina recalled.
For six months they treated Charlee for epilepsy. But when she started tripping on the stairs and having recurrent tremors and shakes, the family renewed testing and discovered a part of her brain was shrinking.
Charlee started having drop, or atonic, seizures, sometimes as many as 200 or 500 a day. "She would just cry for hours at a time. She couldn't communicate or tell us if it hurt but I just know she was in pain," Catrina said.
The family tried numerous medicines and a high-fat, ketogenic diet, recommended for nearly all children with seizures.
Because doctors had not yet diagnosed Charlee, they didn't realize fats were the enemy.
"She was potty trained but days after starting the diet was wetting her pants," Catrina said. "We thought, 'Gosh this seems like it's making her worse,' but we felt it was our last hope."
Charlee's eye doctor first noticed the retinal formations that led to her genetically confirmed diagnosis of Batten disease 21 months after her first seizure. By then Charlee could no longer walk or talk and was nearly blind.
For her the worst part was over — all the blood tests, spinal taps, skin biopsies and brain monitoring.
"She never seemed like she knew something serious was going on because her brain was more like a baby's by the time it got really bad. She never feared losing her life, which is a blessing I guess," Catrina said. "In a way it feels like we lost her two years ago."
Still, the family resolved to make her final moments count.
Last April the Make-A-Wish Foundation flew them to Disney World. "She loved the thrill ride, Splash Mountain, because even though she couldn't see, she could feel the motion in her tummy. She was grinning the whole time," Catrina said.
Family and friends have an open invitation to drop by the house.
"I just wanted them to not have regrets and to be able to come and hold her and say their goodbyes," she said.
Neighbors and members of their LDS church — all "Charlee's Angels" — have donated studio-quality family portraits, an oil painting of Charlee before the seizures, therapeutic massages and food.
Then, in February, she stopped eating and had to be admitted to the hospital.
"Her vitals have declined in the last couple of weeks," reads a Feb. 27 Facebook post by Catrina. "Jeff and I have had an emotional week. We've had a lot of hard talks and hard decisions to make."
Charlee worsened. Her brain stopped communicating with her body and now all the family can do is keep her sedated and comfortable.
On March 4 she smiled when told she could leave the hospital and go home.
She still perks up when she hears her mom's voice. A favorite plush bear that sings the ABC's when you squeeze can coax a smile.
"She's an amazing little girl," Catrina said.
Last Thursday the family summoned close friends and relatives. Charlee's breathing had become shallow. She was gasping for air, looking up at the ceiling and reaching toward something. "I put the oxygen on her and called my husband and said, 'You have to come home. I think we're losing her.' "
She has held on, though, and on Monday lay on the couch, wrapped in her favorite purple blanket with her siblings as they watched TV and played video games.
If she needs oxygen again "we won't be giving it to her," Catrina said through tears.
She has been honest with her children about Charlee's prognosis but tries to keep "things light."
"I try to be strong and stuff but it's hard. You shouldn't have to bury your baby," she said. "Parents talk of a lifetime of epilepsy; I would take epilepsy in a heartbeat. It's all devastating, but to watch your child go from normal to lifeless in a manner of months … there are no words."
Twitter: @KStewart4Trib —
Cannabis for kids
Moved by the plight of children such as Charlee, lawmakers largely have supported allowing their compassionate use of nonintoxicating cannabis oil, but they remain concerned the oil may be abused.
HB105 would give families trial access to the oil under the auspices of research. Only those with intractable epilepsy and written permission from a board-certified neurologist could apply to the Utah Department of Health for a waiver giving them permission to import cannabis oil.
The oil would have to be certified to contain at least 15 percent cannabidiol (CBD), the chemical believed to have anti-seizure properties, and less than 0.3 percent of tetrahydrocannabinol, or THC, the psychoactive chemical that gives marijuana users a high.
Plus, the bill was amended to expire in two years, allowing lawmakers to test its results.
The Senate is expected to amend the bill again to require the health department to work with law enforcement officials to ensure waivers aren't easily forged. In addition, neurologists would have to send their written permission to health officials electronically to avoid fraudulent recommendations. To donate
For information on how to donate to help the Nelsons cover their daughter's medical costs, vist: http://www.charleesangels.org