This is an archived article that was published on sltrib.com in 2013, and information in the article may be outdated. It is provided only for personal research purposes and may not be reprinted.
When Wade Paxman is stressed, he clenches and grinds his teeth.
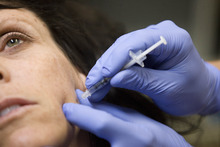
The conventional treatment, mouth guards, protect his enamel but don't ease his jaw pain or crushing headaches. Recently, however, the 53-year-old found relief in a drug most commonly used to rid middle-aged women of unwanted wrinkles: Botox.
"It's just magic. I love it," said Paxman, who drives from Brigham City to Bountiful every six months for treatment. "I'm saving my teeth and enjoying better health. It's as simple as that."
The off-label use of Botox to treat jaw tension and pain is experimental and just catching on in Utah. A few oral surgeons use it therapeutically; Paxman was only able to find one dentist who offers it.
But growing interest in the drug's dental applications is forcing debate over whether dentists should use it cosmetically.
Utah law is vague and says dentists can administer and prescribe drugs "related to and appropriate in the practice of dentistry."
In 2008, the licensing board defined that to include Botox, but only for therapeutic reasons. Cosmetic uses — injecting it for a wrinkle-free brow or smile — are off limits, the board declared.
Utah dentists aren't exactly clamoring to add Botox to their smile makeover repertoire of teeth whitening and veneers. Oral surgeons have free rein to use it.
And, for now, the Utah Dentist and Dental Hygienist Licensing Board isn't inclined to revisit the rules for dentists, despite lobbying this spring by Allergan, the maker of Botox.
"They wanted us to commit to the fact that a general dentist can order Botox and said otherwise we won't sell to dentists, period," said the board's chairman Rich Radmall, a dentist in Ogden. "The board hasn't taken a stand. We're cautious to change anything categorically without knowing the full ramifications."
The dentistry board in Massachusetts approved a policy last March, allowing general dentists to administer botulinum toxins and other injectable wrinkle reducers, called dermal fillers, joining 20 other states with similar rules, according to the American Dental Association (ADA). Key to the decision was growing interest by academics in Boston's dental schools, the ADA says.
Radmall is on the fence. "I imagine there's growing interest in Botox by younger dentists coming out of school. It's kind of like sleep dentistry. Everyone was a little afraid of it, and proceeded with caution. Now sedation is a mainstream tool," he said.
But changing regulations would require further study and legislation, he said. "As a board we talked about there needing to be some kind of training requirement."
Others argue Botox injections are well within a dentist's scope of practice.
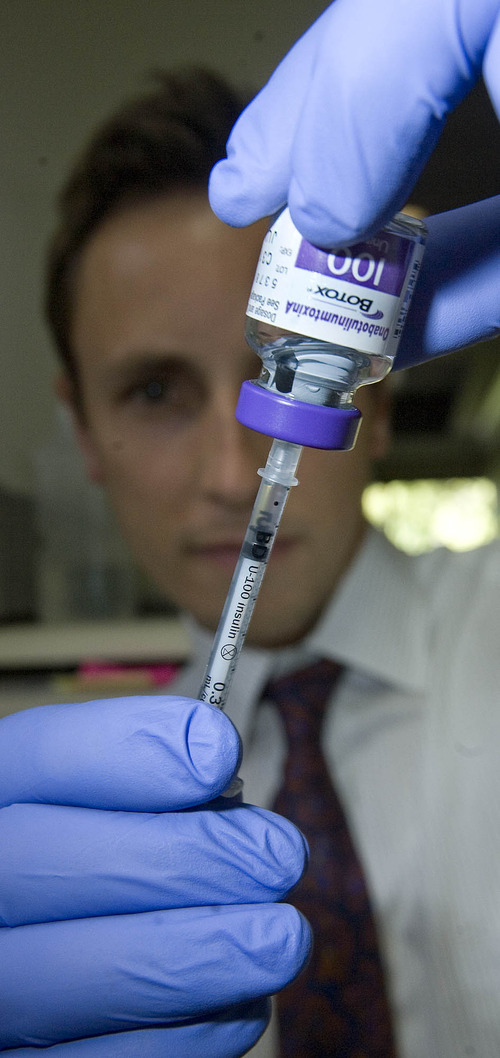
Dentists inject local anesthetic into patients' cheeks and gums. And they're free to administer "Botox Therapeutic," which is the same product in different packaging.
Botox is the same neurotoxic protein that, in large doses, causes botulism, a rare paralyzing illness often linked to food poisoning. In rare cases, it can spread beyond the injection site and cause paralysis, according to the U.S. Food & Drug Administration.
But side effects are generally temporary, since Botox wears off.
"A Botox injection is a Botox injection, whether you're using it to treat pain or reducing wrinkles, it's still the same risk," said Paxman's dentist, Jordan Davis, who underwent a year of oral surgery training in dental school that covered Botox and dermal fillers.
"Our practice is a cosmetic practice, so it would be pretty cool to use dermal fillers to really enhance patients' smiles," he said.
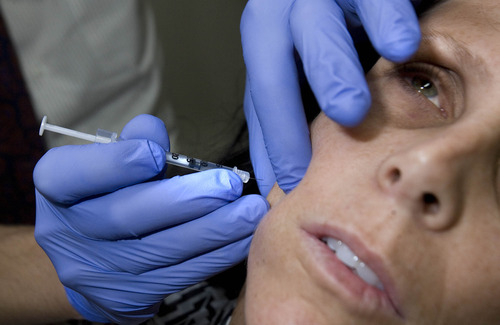
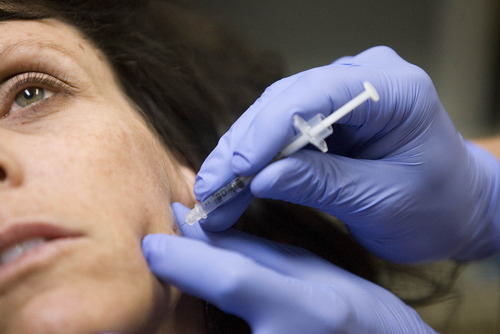
For now, though, he uses Botox on a sparingly few patients with severe jaw clenching and grinding, called bruxism.
Davis gauges the dose, or number of units, according to a patient's size and severity of their grinding, generally injecting the Botox into the jaw and temple.
The drug "tames" the muscles, he said. "I usually start pretty low and have them come back within a few weeks to see how it's working."
Botox won't fix temporomandibular joint disorders (TMJ), such as arthritis or dislocations, but for patients such as Paxman, it's "a blessing," Davis said.
Before Botox, Paxman said he woke nearly every morning with a "bad" headache. "As you can imagine, it's not a good way to live," he said.
His jaw muscles don't feel weak or numb after treatment, he said. "It's not like novocaine."
Davis charges Paxman $10 a unit; the last treatment totalled $450.
"But I'd pay $2,000," Paxman said. "It's hard to describe what a difference it's made for me. It's a quality-of-life issue."
Twitter: @kirstendstewart