This is an archived article that was published on sltrib.com in 2011, and information in the article may be outdated. It is provided only for personal research purposes and may not be reprinted.
Vera Davis was at her home in Kanab on April 13 when she started having chest pains severe enough to send her to the emergency room at her local hospital.
An ultrasound revealed an aortic aneurysm, a balloon-like bulge in the 28-year-old's aorta that threatened her life.
Aneurysms — which can cause serious bleeding and death if they burst — are common and readily repaired in what has become a fairly straightforward surgery.
But her case was anything but routine. Davis has Turner syndrome, a genetic chromosomal disorder that occurs in about 1 in 2,000 newborn girls and can cause heart defects — the leading cause of death for people with Turner's.
But surgeons at Intermountain Medical Center in Murray were able to save Davis with three consecutive surgeries that they described at press conference on Thursday as unprecedented — at least in the combined way that they were performed.
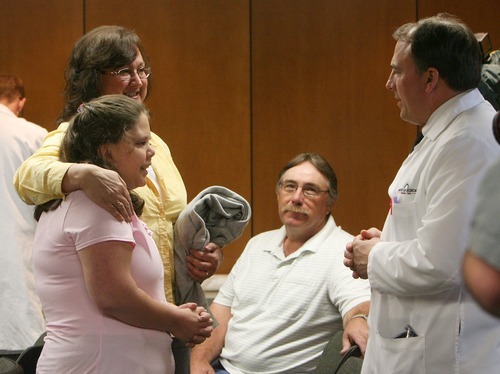
"She is the closest we can get to a modern medical miracle," said cardiovascular and thoracic surgeon John Doty, one of a team of doctors to work on Davis.
Davis had always had a heart murmur, but until the chest pains she wasn't aware of any other heart problems. Due to complications with Turner syndrome, the hospital in Kanab flew her to St. George, where she met with a doctor who got her hooked into the team at Intermountain.
Even today she said it's hard to wrap her head around the gravity of her situation and how lucky she is to be alive. "At 28 you think about your life and your future, not about the possibility that you could die tomorrow," she said.
Davis had unusual branching of the great vessels of the aorta. Her aneurysm had developed a tear and was in danger of rupturing, but due to its location and her unusual anatomy, a traditional approach would have cut off blood flow to her brain or arms.
Doctors, after consulting experts and research papers, decided to break her treatment down into three surgeries. The first, on April 25, involved two surgical teams led by Doty and vascular surgeon Douglas Wirthlin, who worked simultaneously on each side of her body to create two bypasses from the arteries in her neck to the arteries in her arm.
Turner patients have "inherently weak blood vessels," said Wirthlin, who worried that Davis' might rupture when they inserted needles and catheters. But her body responded well, and the surgery was a success.
"The first thing she asked us when she woke up was, 'Did you get something to eat?' " said her mother, 47-year-old Cecilia Tait.
The bypasses created a new path for blood flow while doctors repaired the aneurysm on April 27.
Interventional radiologist Duane Blatter and Wirthlin sewed a tubular endovascular stent-graft inside the aneurysm, which Wirthlin described as inserting a pipe within a pipe. There was little margin for error, said Wirthlin, who explained that if they inserted the stent too far it would have cut off blood flow to Davis' brain.
Blatter then used a catheter to pack the abnormal artery to her right arm with 50 tiny metal coils, which cause the body to form a large blood clot and prevent any blood from flowing back into the aneurysm.
Such coils have been around for decades, but techniques for inserting them are far less invasive. They are permanent and will eventually congeal into a scar.
On May 2, Blatter used more coils to do the same in her left arm and further sealed the aneurysm.
Davis recovered from her surgeries within days and looks forward to camping this summer and finding a job in education.
The Intermountain doctors donated their time and expertise for the expensive procedures and plan to publish their case study. Doty said these techniques have never been used all at once in this way in the United States. There may have been three similar cases worldwide.