This is an archived article that was published on sltrib.com in 2012, and information in the article may be outdated. It is provided only for personal research purposes and may not be reprinted.
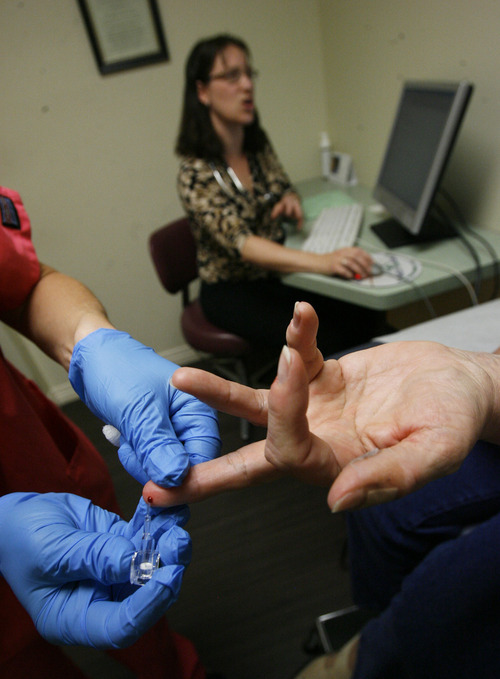
South Jordan -- It's 10 a.m. on a Tuesday and CopperView Medical Center internist Mary Tipton is already an hour behind schedule.
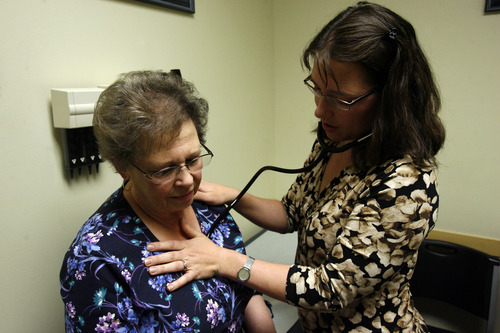
"Dolores, how are you? You look great," she says as she breezes into her next exam, where 69-year-old Dolores Drayer waits for what she hopes is the happy conclusion to a year of hard work.
Since her diagnosis last summer with diabetes, Drayer has dropped 40 pounds. She eats differently and rides a stationary bike for an hour daily, which has given her more energy and helped lower her blood pressure. Today's blood test will tell whether she's disease-free.
"I hate this part," says the Herriman woman, wincing as a nurse pricks her middle finger to draw blood. "Contrary to popular belief, you don't stop being a baby when you turn 60."
Visiting the doctor isn't fun. It's expensive, inconvenient, uncomfortable and only part of the healing equation. The ingredients for wellness, experts say, break down like this: 50 percent behavior, 20 percent genetics and 20 percent environment — leaving doctors like Tipton a 10 percent window for making a difference.
Yet policymakers look to medical professionals to solve an epidemic of heart disease, obesity and diabetes that is drowning the country in debt and killing more people than infectious diseases. Clinics, specialists and hospitals that improve their care will be paid more under changes driven by federal health reform. Those that don't will earn less.
For time-starved primary care physicians, says Tipton, that means finding the sweet spot for intervention: the right therapy at the right time for the right person. And it all starts with technology.
Tipton's clinic is among 62 in the Salt Lake City area taking part in the "Beacon Community" project, an experiment leveraging electronic health records to improve care for 50,000 Utahns with Type II diabetes. The project is funded with part of a $16 million federal grant and overseen by the Utah-based non-profit advisory group, HealthInsight.
"Payment for performance is not going away. I want our clinic to be at the forefront," said Tipton.
—
Carrots and sticks — for doctors. • Traditionally, doctors have been paid for services, not for how well they serve patients. That's changing, largely due to new incentives and penalties under Medicare.
Medicare is giving bonuses to providers who convert to computerized medical records, which promise greater efficiency, patient safety and the ability to produce data to improve care. In 2015, those carrots turn into sticks and technophobes who resist will see a 1 percent drop in their Medicare payments. After that, the penalty increases by a percentage point each year for five years.
That may not amount to much for family clinics, where 20 percent of their average $500,000 revenue stream comes from Medicare. Under that scenario, a 1 percent drop in pay equals about $1,000.
But 1 percent can add up fast for large hospitals and doctors who specialize in senior care. And these penalties are just the beginning.
State Medicaid programs and private insurers are also devising ways to reward providers for meeting certain quality goals, such as annually screening diabetics for bad cholesterol and high blood pressure.
Technology alone won't move the needle, said Sarah Woolsey, a Utah physician and medical director for the Beacon project. "But it's the building block. If we don't have data, how do we measure outcomes?"
It's America's public health quandary.
Two-thirds of adults and one-third of the country's children are overweight or obese. Diabetes alone accounts for $1 of every $3 of Medicare spending. One of three children born today will have the disease at some point in their lives.
Properly managed, these conditions can be slowed or reversed. The question is how much onus to place on health professionals.
—
Opening eyes with data. • Payment for performance has been criticized as unfair, because so much of our health rests on decisions we make outside the doctor's office, about what we eat and how we sleep and exercise.
One study by the Rand Corporation suggested it could hurt medical practices that cater to populations at greater risk for chronic disease — the poor, racial and ethnic minorities — further widening health disparities.
Small rural clinics and stand-alone practices like Tipton's especially struggle to meet the mandates because they lack the computing power of major health chains. She and a partner started it six years ago and it has grown to employ five doctors and seven mid-level providers.
But she feels the pressure of new regulations and billing challenges that compete for her already scarce time.
"Quality care is probably the goal of every doctor who takes the oath. Then life comes at you and you have a system and a workflow that keeps impeding progress," she said.
The Beacon project seeks to remove those impediments. One of the goals is to get doctors wired enough to share patient data via a data superhighway called the cHIE, or Clinical Health Information Exchange. Another is to upgrade their electronic medical records to function more like databases.
Tipton's clinic was among 30 targeted for more intensive help. "We're seeing the biggest leap with this group, because frankly, they had the farthest to go," said Woolsey.
CopperView's paperless system was "mainly was just a replacement for paper charts," Tipton said. Like most doctors, she treated patients when they got sick or needed a regular check-up, surfing through digital notes about previous appointments.
There was no automated way, for example, to search for patients with high cholesterol or high blood pressure, or to reach out to those who were overdue for a hemoglobin A1c test, which gives a six to 12-week average of a person's blood sugar control.
"We needed to create a system to make quality care easier to do than not to do," Tipton said.
HealthInsight's first data pull from Tipton's improved computer system was an eye-opener.
About 30 percent of the 1,800 diabetics treated at CopperView were overdue for their A1c test. Fewer than half had their blood sugar under control.
Even fewer showed they had been in for an eye exam, in part because the clinic doesn't do those exams and had no record of the results. Diabetes is the leading cause of blindness in adults.
CopperView wasn't alone. Its numbers track or slightly exceed state and national averages.
—
'Making a difference.' • A well-timed A1c was exactly what tipped the scales for Drayer. The retiree wasn't showing signs of diabetes, but Tipton ordered the test as a precaution.
"There's nothing like finding out you have a disease to make you lose the weight you've been carrying around for 25 years," said Drayer. "This year has transformed my life. You take so much for granted when you think you're well."
HealthInsight created a web portal where clinics can monitor their own health, comparing themselves to other providers on eight standards of diabetes care.
Not all patients are as self-motivated as Drayer.
Some face circumstances beyond their control, said Elisa Scherzinger, nurse manager at the Utah HealthCare Institute, a family practice operating out of St. Mark's Hospital. Some are poor and uninsured, in depression or in denial. Others are new to this country with language barriers and unusual diets, she said.
Scherzinger oversees a team of nurses, dieticians and care managers who reach out to such patients by any means — text, email, phone and a web portal where patients can submit questions. They're trained to listen well during motivational interviewing and, when necessary, refer patients to services in the community – something social workers and hospital discharge planners do, but few clinics.
"Staff really feel empowered because they're operating at the top of their scope of practice," said Scherzinger "They feel like they're making a difference in peoples' lives."
—
Watching for the payoff. • Two years in and the Beacon project is showing results.
High performing clinics like Tipton's have seen a 20 percent increase in patients getting their needed health screens, and a 10 percent jump in patients with control of their blood sugar, cholesterol and blood pressure.
There have also been gains in the number of patients receiving medical attention for kidney disease, eyesight problems and other health risks tied to diabetes.
Whether this will pay off in lower health costs by reducing complications, such as blindness and amputations, remains to be seen.
But Tipton is hopeful. CopperView is near its goal of having 90 percent compliance on A1c testing.
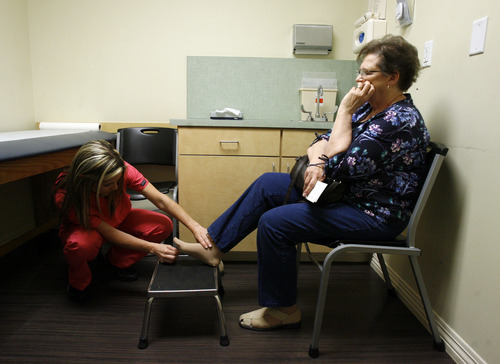
While they await Drayer's test results, Tipton reviews her prescriptions and checks her legs and feet for signs of poor circulation.
Her blood pressure is higher than usual today, which could be nerves.
Drayer tells her she is sticking with her diet, but hasn't been biking as much because her hip is bothering her. She has stopped losing weight, which is frustrating.
"But you're maintaining your weight," Tipton says reassuringly.
A nurse enters with Drayer's test results: 5.9 on a scale of 5 to 11.
"That's normal. You're no longer in the diabetic range," says Tipton. "We'll see you in six months."
kstewart@sltrib.comTwitter: @kirstendstewart —
A prescription for health
Fifth in an occasional series
About this series
Federal health reform has drawn increased scrutiny to what's broken in health care and has inspired new thinking on how to fix it. This story is part of an occasional series on innovation among Utah's hospitals, clinics and insurance companies. —
A prescription for health —
See these previous stories in the Tribune's series:
Can better care cut costs for Utah's priciest Medicaid patients?